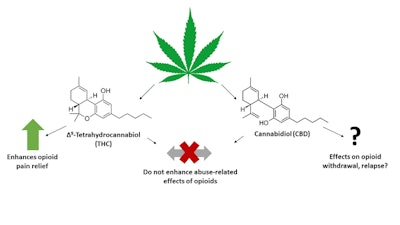
Findings from a new animal study suggest that cannabidiol (CBD) and tetrahydrocannabinol (THC) might be safe for use with opioid pain relievers. Although more studies are needed, the results suggest that these compounds might be a low-risk way to reduce the dose of opioids needed to relieve pain.
“There is intense interest in using medical marijuana in patients with chronic pain because compounds in marijuana like CBD and THC may produce pain relief themselves or enhance the pain-relieving effects of opioids,” said Lawrence Carey, PhD, a postdoctoral fellow at the University of Texas Health Science Center, San Antonio. “This means people could potentially use lower doses of opioids and still get relief from pain. Taking less pain medication could also lead to a lowered risk of addiction or physical dependence to opioids.”
The researchers found that CBD and THC do not enhance the rewarding effects of opioids. This means that these compounds may not increase the risk for addiction when used in conjunction with opioids.
Carey will present the new research at the American Society for Pharmacology and Experimental Therapeutics annual meeting during the Experimental Biology (EB) 2022 meeting, to be held April 2–5 in Philadelphia.
In the new study, the researchers gave rhesus monkeys the opportunity to choose a food reward or an injection of the opioid fentanyl. They then tested whether CBD, THC or mixtures containing both compounds affected the number of times monkeys selected fentanyl over food. They found that a wide range of doses of CBD or THC both alone or in a mixture did not increase or decrease the number of times they selected fentanyl.
“Giving the animals the opportunity to choose between a drug injection and a food reward helped us to somewhat replicate choices a human drug user may face, such as whether to spend money on drugs or food,” said Carey. “Having the option of responding for food is also useful for studying drugs like THC that produce sedative effects. It helps demonstrate the animal is reallocating behavior from drug to food choice instead of simply shutting down response for a drug due to sedation.”
The researchers are now conducting other studies to assess whether CBD and THC can decrease signs of opioid withdrawal and relapse.
“A big reason why people continue to take opioids after they become addicted is the appearance of withdrawal symptoms,” said Carey. “We are using what we learned from this study to determine whether these doses — which didn’t alter choice for food or drug rewards — may help relieve opioid withdrawal or decrease relapse and drug seeking behavior following periods of abstinence.”
The researchers caution that opioid use disorder is a complex disease and there are many factors to consider when developing a drug to treat it. Although this study indicates that THC and CBD do not increase the rewarding effects of opioids, they say that before applying these findings to people, it will be necessary to determine whether these treatments alter other pathological processes involved with opioid use and to better understand any risks that may be associated with their use.






















